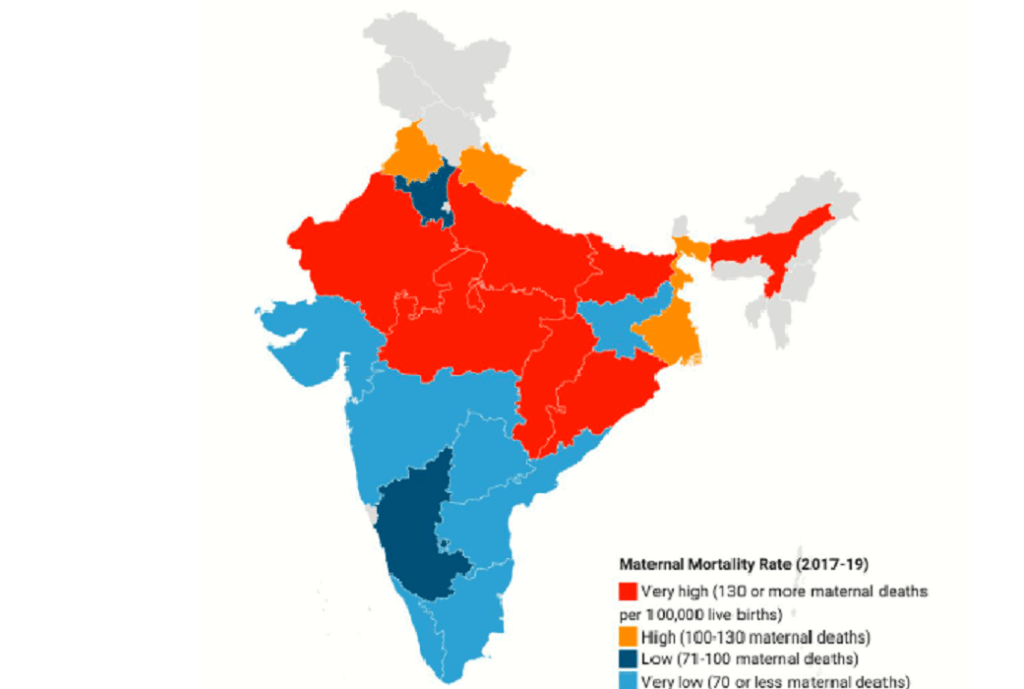
A recent survey reveals that West Bengal’s maternal mortality ratio (MMR) now stands at 104 deaths per 100,000 live births for the period 2021-23, well above the national average of 88. This alarming figure places Bengal on par with Bihar, but behind several other states including Jharkhand, Rajasthan, Uttarakhand, Haryana, and Punjab.
MMR measures the number of mothers who die due to complications from pregnancy or childbirth per 100,000 live births. The data shows that Bengal has slipped from earlier times when its MMR was below the national average. For instance, in 2007-09 Bengal’s MMR was 145, compared to a national average of 212. By 2010-12 it dropped to 117; later, by 2016-18, it reached a lower value as well. But since the years 2017-19, Bengal’s MMR has consistently been above the national average.
States such as Kerala and Andhra Pradesh have achieved much better outcomes, with MMR of approximately 30. Bengal’s performance in maternal health has deteriorated after the COVID-19 pandemic, according to officials and experts.
Several reasons are being cited for this decline. Direct causes of maternal death include postpartum hemorrhage, pre-eclampsia and hypertensive disorders, infections during or after pregnancy, and complications from unsafe abortions. Indirect causes such as pre-existing medical conditions—like hypertension or diabetes—that are not properly managed before and during pregnancy are also major contributors.
Geographically, rural and small-town areas are disproportionately affected. Many women from lower income groups often ignore or are unable to diagnose and treat medical conditions before pregnancy. Antenatal care gaps, lack of awareness, insufficient healthcare infrastructure, and social neglect factor into the risks.
West Bengal’s health department claims that institutional deliveries are now nearly universal—around 99% of childbirths happen in a facility. However, officials acknowledge that there are still “grey areas” in prenatal health monitoring and management of at-risk pregnancies. Maternal death audits—which examine each case to identify medical and social causes—were introduced over a decade ago. There are concerns about whether these audits are now being consistently implemented.
As things stand, while the decline in national maternal deaths continues, Bengal’s rate raises concerns over healthcare delivery, outreach, and equity. Unless systemic gaps are addressed—especially in rural areas, preventive care, and monitoring—Bengal risks falling further behind in maternal health outcomes.